

Your body sends clear, measurable signals in the days before and during ovulation, the phase in your cycle when pregnancy is possible. The most reliable physical signs include a change in cervical mucus to a clear, slippery consistency, a slight rise in basal body temperature, and mild one-sided pelvic pain. Recognising these signs helps you identify your fertile window accurately so you can time conception or plan around it.
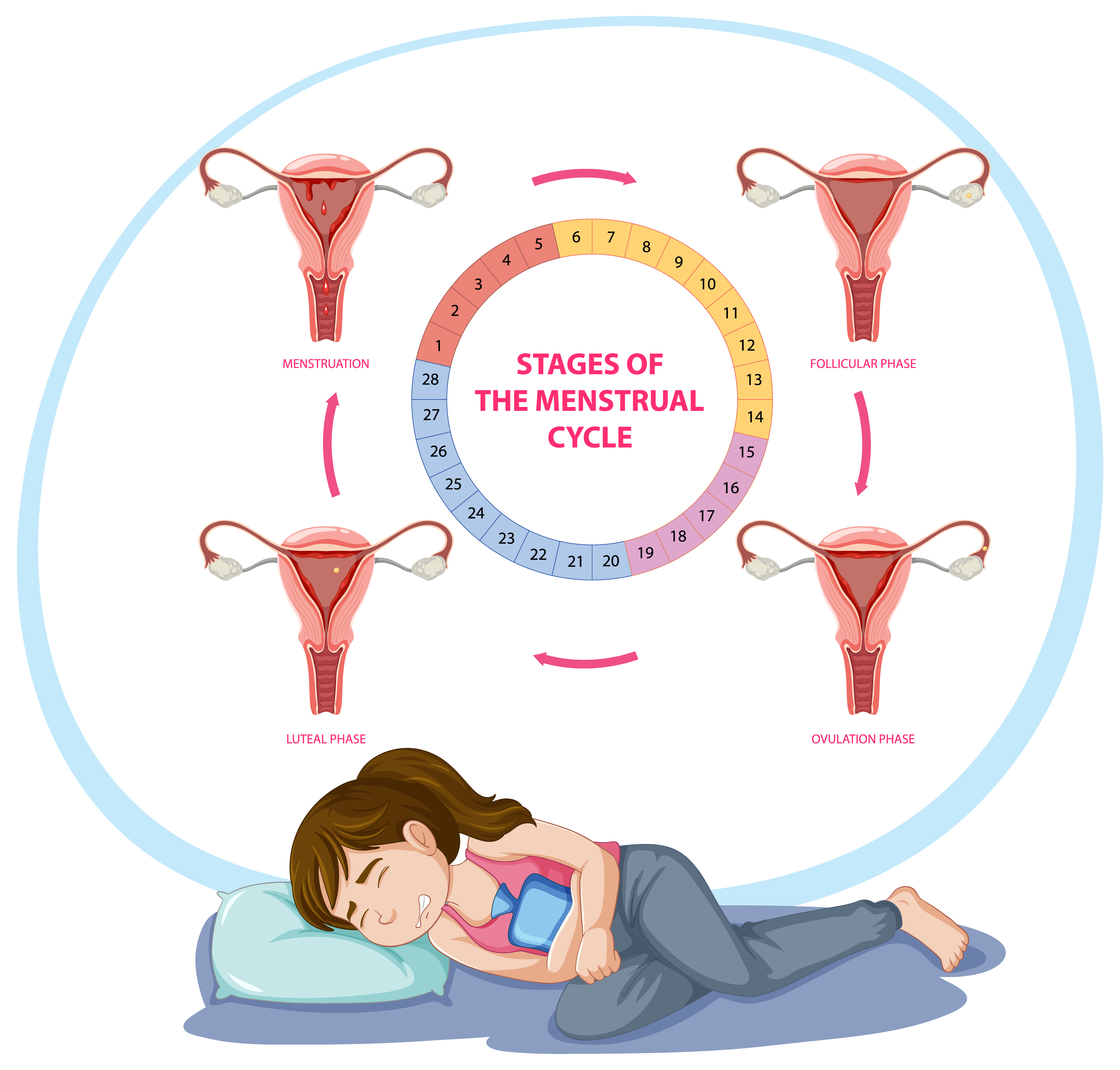
Ovulation is the release of a mature egg from one of your ovaries, triggered by a surge in luteinizing hormone (LH). It occurs once per menstrual cycle, typically around day 14 of a standard 28-day cycle, though this varies depending on cycle length. The egg survives for only 12 to 24 hours after release. Sperm, however, can survive inside the female reproductive tract for up to five days. This creates a fertile window of approximately six days each cycle, the five days before ovulation plus the day of ovulation itself.
For many Indian women, the conversation around fertility only begins when conception has not happened despite trying for several months. By that point, months of potential fertile windows have already passed unrecognised. Your cycle is actively communicating with you every month through hormone-driven physical changes that are consistent, measurable, and learnable. Understanding them is not just useful for women trying to conceive; it is equally relevant for those who want to establish a baseline of their reproductive health, identify irregularities early, or simply know their bodies better. Fertility awareness is not a workaround; it is a clinical tool used by fertility specialists alongside blood tests and ultrasounds to map the hormonal patterns that govern your cycle.
Not every woman experiences all seven signs, and their intensity varies. The more of these you track simultaneously, the more accurately you can pinpoint your fertile window.
This is the single most reliable physical sign of fertility. In the days leading up to ovulation, cervical mucus transitions from dry or thick and white to clear, slippery, and stretchy, often compared to raw egg whites. This consistency allows sperm to survive and travel toward the egg. Once ovulation has passed, mucus returns to a thicker, sticky consistency. Checking cervical mucus takes no equipment and can be done daily.
Basal body temperature is your resting temperature, measured the moment you wake up before getting out of bed, eating, or drinking. In the days just before ovulation, BBT drops slightly. It then rises by approximately 0.2 to 0.5 degrees Celsius after ovulation occurs, driven by progesterone, a hormone your body releases to prepare the uterus for possible pregnancy. This rise confirms that ovulation has already happened. To use BBT accurately, you need a basal thermometer and consistent daily tracking over several cycles to identify your personal pattern.
Around 40% of women experience a distinctive lower abdominal or pelvic pain on one side during ovulation. This is called Mittelschmerz, German for 'middle pain'. It typically lasts from a few minutes to a few hours and corresponds to the rupture of the follicle and the release of the egg. The side of the pain can alternate with each cycle, depending on which ovary is active. It is a useful secondary confirmation sign, not a primary tracking method on its own.
Hormonal shifts around ovulation, particularly the LH surge (the sharp rise in luteinizing hormone that triggers egg release), can cause breast tissue to feel tender, fuller, or more sensitive. This sign is common but not specific to ovulation alone, as it also occurs premenstrually. Use it as a supporting indicator alongside cervical mucus and BBT changes rather than in isolation.
A rise in estrogen, the hormone that builds up in the days before ovulation and drives egg maturation, is associated with a measurable increase in sexual drive in many women. This is a biological mechanism that evolved to maximise the potential for conception during the fertile window. If you notice a cyclical pattern of increased sexual interest that repeats month to month, this is a useful fertility signal worth tracking.
Some women experience very light spotting, a few drops, or a faint pink or brown discharge at ovulation. This mid-cycle bleeding occurs when the follicle (the fluid-filled sac containing the egg) ruptures, and estrogen briefly drops before progesterone takes over. Think of it as a brief hormonal handover between the two phases of your cycle. It is typically lighter than a period and lasts one to two days. If mid-cycle bleeding is heavier or more frequent, it warrants investigation by a gynaecologist.
Research has found that women near ovulation may have a temporarily heightened sense of smell, particularly for male pheromones. Mild abdominal bloating is also commonly reported due to water retention driven by rising estrogen, the same hormone responsible for the mucus changes you notice around your fertile window. Both are secondary signs useful for pattern recognition over multiple cycles, but not reliable in isolation for pinpointing ovulation day.
Treat the underlying cause: Thyroid disorders, PCOS, and high prolactin all respond well to medical treatment, and in many cases, treating the root cause is all that is needed to restore regular ovulation naturally.
Self-tracking is a useful first step, but it has clinical limits. If any of the following apply to you, a consultation with a fertility specialist rather than a general gynaecologist is the appropriate next step.
If you are in Bangalore, Delhi, Mumbai, Hyderabad, Chennai, Pune, or Chandigarh, Cloudnine Fertility's specialists offer a dedicated fertility assessment, including a hormonal panel, ultrasound, and a personalised cycle analysis to give you a clear picture of your ovulatory health. Book a consultation at your nearest Cloudnine Fertility centre.

Evidence consistently shows that cycle tracking combined with timed intercourse improves conception rates compared to untracked attempts. The figures below draw on published reproductive medicine research:
If you have been tracking your ovulation signs and still have not conceived, the next step is a clinical fertility assessment, not more months of waiting. Cloudnine Fertility's specialists in Bangalore, Delhi, Mumbai, Hyderabad, Chennai, and Pune combine hormonal testing, ultrasound monitoring, and cycle analysis to identify exactly what is happening and what to do next. Book your fertility assessment today.
Also read:
→ How to use ovulation test kits to detect your fertile window
→ What is AMH testing and what does your result mean for fertility?
→ Follicular monitoring: how ultrasound tracking confirms ovulation
